How Is MR-Guided Focused Ultrasound Doing Today: Essential Update
This important update shows that MR-guided Focused Ultrasound (MRgFUS) is rapidly advancing, offering non-invasive treatment options for various conditions and becoming more accessible in clinical practice.
Ever heard of a treatment that uses sound waves to help people without any cutting or needles? That’s pretty cool, right? MR-guided Focused Ultrasound, or MRgFUS for short, is that amazing technology. It’s like a high-tech, super-precise way to treat problems in the body. Lots of people are curious about it and wonder if it’s just science fiction or if it’s actually helping real patients today. We’re going to break down exactly how MRgFUS is performing right now, what it can do, and what makes it so special. Get ready to learn about a truly innovative medical advancement!
What is MR-Guided Focused Ultrasound (MRgFUS) Anyway?
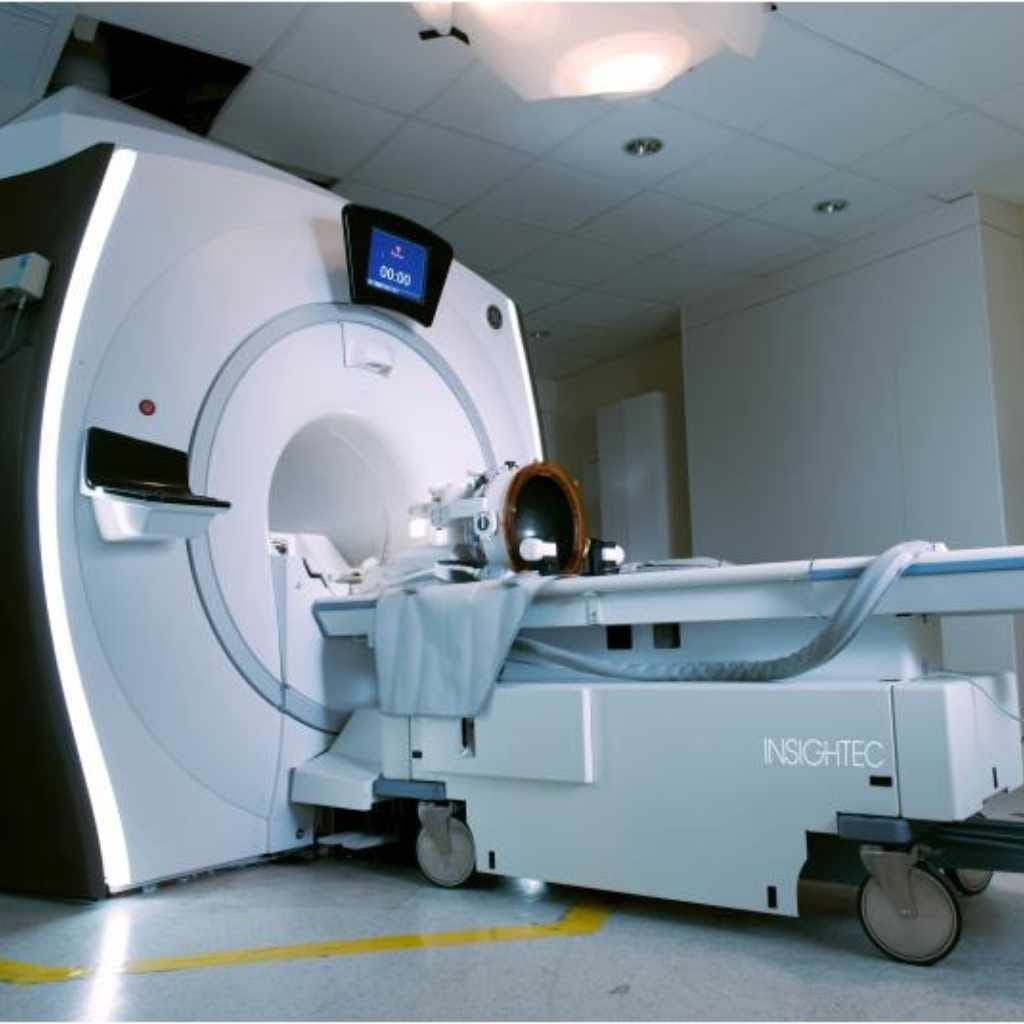
Imagine using invisible beams of sound, focused like a magnifying glass on sunlight, to heat and destroy tiny, unwanted cells inside your body. That’s the basic idea behind MRgFUS. It combines two powerful technologies: Magnetic Resonance Imaging (MRI) and High-Intensity Focused Ultrasound (HIFU).
- MRI’s Role: The MRI scanner acts like your eyes. It creates detailed, real-time images of the inside of your body. This allows doctors to see the specific area they need to treat and make sure the ultrasound beams are going exactly where they should. It also helps them monitor the temperature and the effects of the treatment as it happens.
- HIFU’s Role: The Focused Ultrasound part is like the precision tool. It uses special ultrasound transducers (these are like speakers for sound waves) to generate high-energy sound waves. These waves are carefully aimed at a very small spot. When they all meet at that spot, they create heat, which can destroy or inactivate cells.
The magic happens when these two work together. The MRI guides the HIFU beams precisely to the target, making sure healthy tissue around it is left untouched. This means it can treat deep inside the body with incredible accuracy, avoiding the need for surgery.
How Is MRgFUS Doing Today? An Essential Update
So, how is this technology actually performing “today”? The answer is: better than ever! MRgFUS is moving from research labs into more widespread clinical use. It’s not just a concept anymore; it’s a proven treatment option for several conditions.
Expanding Treatment Applications
Originally, MRgFUS was approved for treating essential tremor and uterine fibroids. But today, its applications are growing rapidly. Doctors are using it, or are in advanced stages of research for, conditions like:
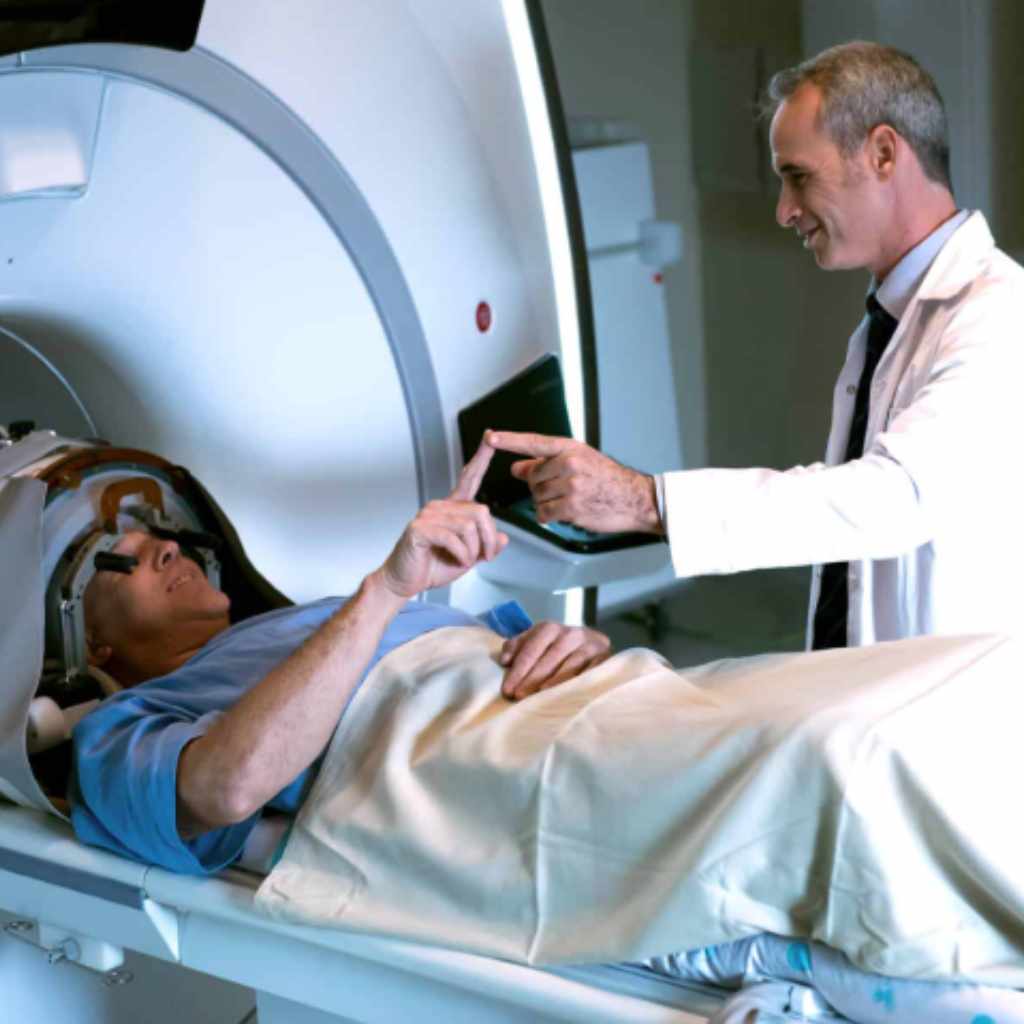
- Essential Tremor: This is one of the most established uses. MRgFUS can significantly reduce the shaking in hands for people with essential tremor, often with immediate results and minimal downtime.
- Uterine Fibroids: For women suffering from these non-cancerous growths in the uterus, MRgFUS offers a non-invasive alternative to surgery, helping to relieve symptoms like heavy bleeding and pain.
- Prostate Cancer: MRgFUS is showing promise as a treatment for localized prostate cancer. It can be used to precisely target and destroy cancerous tissue while sparing surrounding healthy areas, potentially reducing side effects like those associated with traditional surgery or radiation.
- Osteoarthritis (Knee): Early studies are showing that MRgFUS can help reduce pain and improve function in patients with severe knee osteoarthritis by targeting and modifying specific nerves around the joint.
- Neuropathic Pain: Research is exploring its use to treat chronic pain caused by nerve damage, by ablating specific nerve pathways.
- Parkinson’s Disease: Similar to essential tremor, MRgFUS is being investigated for its ability to target specific brain regions involved in Parkinson’s symptoms.
Technological Advancements
The technology itself is also getting smarter and more efficient. Newer systems offer:
- Faster treatment times.
- Improved visualization and targeting capabilities.
- More sophisticated feedback mechanisms to ensure safety and efficacy.
- The ability to treat larger or more complex targets.
These improvements mean that MRgFUS is becoming a more attractive option for both patients and healthcare providers.
Why is MRgFUS Gaining Traction? The Key Benefits
When we talk about “how is MRgFUS doing today,” a big part of the story is why it’s becoming more popular. The advantages are significant:
Non-Invasive Nature
This is the biggest selling point. MRgFUS treats conditions from outside the body. There are no incisions, no scalpels, and no stitches. This means:
- Reduced risk of infection.
- Minimal scarring.
- Shorter hospital stays or even outpatient procedures.
- Faster recovery times for patients.
High Precision and Safety
The MRI guidance ensures that the ultrasound energy is delivered only to the intended target. This:
- Protects surrounding healthy tissues from damage.
- Minimizes side effects that can be common with other treatments.
- Allows for treatment of targets deep within the body without affecting overlying structures.
Immediate and Long-Lasting Results
For many applications, patients experience relief immediately after the procedure. For example, tremor symptoms often lessen during the treatment itself. For conditions like fibroids or early prostate cancer, the therapeutic effects continue to develop over time.
Outpatient Convenience
Many MRgFUS procedures can be performed on an outpatient basis. This means patients can go home the same day, avoiding the disruption and cost of an overnight hospital stay. This is a huge win for patient convenience and reduces the burden on healthcare systems.
Repeatability
If needed, MRgFUS treatments can often be repeated. This offers flexibility for managing chronic conditions or cases where a single treatment might not be sufficient.
The Science Behind the Sound: How it Works in Detail
Let’s delve a little deeper into the physics and technology that make MRgFUS possible. Understanding this can help appreciate its sophistication.
Focused Ultrasound Energy
Focused ultrasound works by directing multiple beams of ultrasound energy. These beams are emitted from an array of transducers and converge at a single point deep within the body. At this focal point, the individual beams combine their energy, significantly increasing the intensity and causing a therapeutic effect.
| Ultrasound Beam Property | Effect at Focal Point | Effect Outside Focal Point |
|---|---|---|
| High Intensity | Achieved through convergence of multiple beams. | Low intensity, safe for surrounding tissues. |
| Thermal Effect | Rapidly heats tissue to temperatures (above 55°C or 131°F) sufficient for cell ablation. | Negligible heating, maintaining normal tissue temperature. |
| Mechanical Effect (Cavitation) | Can occur, leading to cell disruption or microbubble formation. | None. |
Thermal Ablation
The primary mechanism for most MRgFUS treatments is thermal ablation. When the focused ultrasound waves concentrate at the target, the tissue temperature rises rapidly. This heat causes:
- Denaturation of proteins: Proteins essential for cell function are damaged, leading to cell death.
- Coagulation necrosis: Cells are destroyed and replaced by scar tissue.
The MRI scanner continuously monitors the temperature in real-time using special MRI thermometry techniques. This allows the physician to precisely control the heating process, ensuring the target is adequately treated without overheating nearby structures. For more on MR thermometry, the MRIsafety.com resource offers excellent insights into ensuring patient safety during these procedures.
MR Guidance and Control
The MR scanner is crucial for several reasons:
- Treatment Planning: Doctors use MRI to identify the precise target, define its boundaries, and plan the optimal trajectory for the ultrasound beams.
- Real-time Monitoring: Dynamic MRI sequences provide live images of the treatment area, allowing the physician to track the position of the ultrasound focus and see the immediate effects of the treatment, such as tissue heating or ablation.
- Temperature Mapping: Advanced MRI techniques can measure tissue temperature, providing direct feedback to the operator to adjust the energy delivery and prevent overheating.
- Safety Checks: MRI helps identify anatomical landmarks and potential contraindications to ensure the procedure is safe.
This integrated approach of real-time imaging and therapeutic energy delivery is what makes MRgFUS such a powerful and safe technology.
Current Challenges and Future Outlook
While MRgFUS is doing remarkably well, like any emerging technology, it faces some challenges. Addressing these is key to its continued growth and widespread adoption.
Accessibility and Cost
MRgFUS systems are sophisticated and expensive. This means:
- Availability is currently limited to specialized centers.
- The cost of the procedure can be a barrier for some patients and healthcare systems, although it’s important to consider the potential long-term savings from reduced hospital stays and fewer complications.
- Wider insurance coverage is still being established for some of its newer applications.
Training and Expertise
Operating an MRgFUS system requires specialized training for physicians and technical staff. This includes understanding:
- MRI physics and safety protocols.
- Focused ultrasound technology.
- Anatomy and surgical planning.
- The specific treatment protocols for various conditions.
As more centers adopt the technology, the need for robust training programs, like those often facilitated by institutions such as the HIFU Education & Training Foundation, becomes increasingly important.
Research and Development
While progress is rapid, ongoing research is vital to:
- Expand indications to new diseases.
- Improve existing treatment techniques.
- Develop new therapeutic mechanisms beyond thermal ablation.
- Conduct larger clinical trials to gather more data and confirm long-term outcomes.
Reimbursement Landscape
For any new medical technology to truly become standard of care, favorable reimbursement from insurance providers is essential. For MRgFUS, this process is ongoing as more evidence of its effectiveness, safety, and cost-effectiveness is gathered.
The Future of MRgFUS
The outlook for MRgFUS is incredibly bright. Experts predict that as the technology matures and costs decrease, it will become a mainstream treatment option for a variety of conditions. We can expect to see:
- More widespread adoption in hospitals and treatment centers.
- New applications for diseases currently difficult to treat non-invasively.
- Integration with other treatment modalities for synergistic effects.
- Continued innovation in transducer design, imaging techniques, and treatment planning software.
The trend is clear: MRgFUS is not just “doing okay”; it’s actively shaping the future of minimally invasive medicine.
FAQ Section
What kind of conditions can MRgFUS treat?
MRgFUS is currently used for essential tremor, uterine fibroids, and is expanding into prostate cancer, osteoarthritis pain, and neuropathic pain. More applications are being researched.
Is MRgFUS painful?
The procedure itself is generally well-tolerated because it’s non-invasive. Patients may feel warmth at the treatment site, and their comfort is monitored throughout. Local anesthesia or conscious sedation is often used.
What are the side effects of MRgFUS?
Side effects are typically minor and temporary, often related to the treated area. For example, patients might experience temporary fatigue, skin redness, or mild pain. Because it’s so precise, serious side effects are rare.
How does MRgFUS differ from regular ultrasound used for imaging?
Regular ultrasound uses low-intensity sound waves for imaging. MRgFUS uses high-intensity focused sound waves that are concentrated to generate heat and destroy tissue, guided by MRI scans.
How long does an MRgFUS procedure take?
Treatment times vary depending on the condition and the size of the target area, but they typically range from 1 to 3 hours.
Is MRgFUS suitable for everyone?
No, it’s not suitable for everyone. Factors like the exact location and size of the target, the patient’s medical history, and the presence of implanted medical devices can affect eligibility. A doctor will determine if it’s the right option.
What is the recovery like after MRgFUS?
Recovery is usually quick because there are no incisions. Many patients can resume normal activities within a day or two. Some might experience mild soreness or swelling in the treated area for a short period.
Conclusion
So, to answer the big question: “How is MR-guided Focused Ultrasound doing today?” It’s doing exceptionally well! This innovative technology is rapidly evolving, proving its value as a safe, effective, and non-invasive treatment option for an increasing number of medical conditions. From reducing tremors to treating tumors and managing pain, MRgFUS is making a real difference in patients’ lives by offering a path to healing without surgery. While challenges like accessibility and cost remain, the progress in technology, expanding applications, and growing body of clinical evidence paint a very promising picture. MRgFUS is not just a marvel of modern medicine; it’s becoming a vital tool in its arsenal, offering hope and improved outcomes for many.